Gram-positive organisms exhibited a high rate of sensitivity
to levofloxacin (97.6%), ciprofloxacin (95.43%), and
chloramphenicol (90.74%) and exhibited low sensitivity
(1.2%) and strong resistance (98.2%) to erythromycin.
Gram-negative bacteria exhibited a high degree of sensitivity
to levofloxacin (96.02%), tobramycin (94.12%), ciprofloxacin
(92.75%), and chloramphenicol (83.45%). Both Grampositive
and Gram-negative bacteria were sensitive to
levofloxacin, with an average effective rate of 96.81%.
A total of 359 cases (181 boys, total 241 eyes; 178 girls,
total 252 eyes; total 493 eyes) were included in this study.
Of these, 261 had unilateral infection and 116 had bilateral
infection. The cases were divided into two groups (children
3–6 months of age, 276 eyes; 7–12 months of age, 217 eyes).
Among children from 3–6 months of age, the 1-time success
rate of nasolacrimal duct probing alone was 95.65% and the
1-time success rate of probing combined with nasolacrimal
duct injection of levofloxacin ophthalmic gel was 97.1%
(no statistical significance,
χ2 =0.104,
P=0.747>0.05). Among children from 7–12 months of age, the 1-time success rate
of nasolacrimal duct probing alone was 88.24% and the
1-time success rate of probing combined with nasolacrimal
duct injection of levofloxacin ophthalmic gel was 96.52%
(statistical significance,
χ2 =5.435,
P=0.02<0.05). The 1-time
success rate for simple nasolacrimal duct probing alone
was significantly higher in children from 3–6 months of
age than for those from 7–12 months of age (statistical
significance,
χ2 =4.651,
P=0.031<0.05). The 1-time success
rates of combination therapy with nasolacrimal duct
injection of levofloxacin ophthalmic gel showed no different
between the two groups (no statistical significance,
χ2 =0.000,
P=1.000>0.05) (Tables 2-5).
Discussion
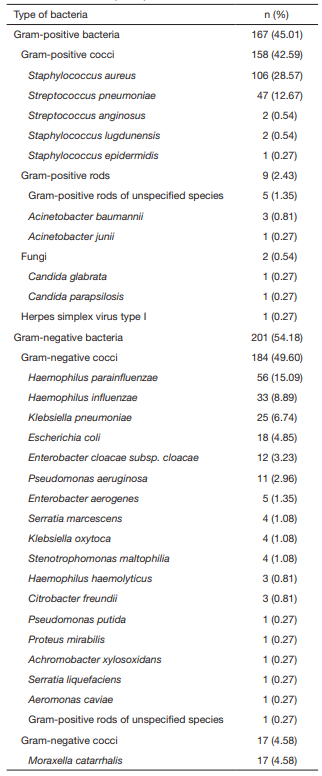
We obtained bacteria cultures of lacrimal sac secretions
of children with dacryocystitis. Of the children whose
secretions were cultured, 75.1% tested positive for
pathogenic bacteria. The most common pathogen
identified was Staphylococcus aureus, followed by Haemophilus
parainfluenzae and Streptococcus pneumoniae. Susceptibility
testing results demonstrated that levofloxacin was the most
sensitive drug for both G− and G+ bacteria.
The distribution of pathogenic bacteria in children with
dacryocystitis shows regional differences. Sun
(22) reported
that G+ strains were the most abundant pathogenic bacteria
(74.5%) in children with dacryocystitis in Shenyang,
although our results differed. The disparity may be due to
different locations that vary in climate; the study by Sun took
place in Northern China, whereas our facility is located in
Southern China. In addition, Sun reported that coagulasenegative
Staphylococcus is the most common pathogenic
bacteria, followed by
Staphylococcus aureus. Our results show
that
Staphylococcus aureus has become the primary pathogenic
bacteria causing dacryocystitis in young children.
Staphylococcus aureus is the most common pathogenic
bacteria for human suppurative infections; as a conditional
pathogenic bacterium, it is often present in the oral cavity,
nasopharynx, palpebral conjunctiva, urethral canal, and
intestinal mucosa. The immune system in young children
is immature, and their tears are deficient in IgA and IgM.
In addition, their lacrimal gland secretion function is not
perfect and their lacrimal duct is not smooth as well as their
bacteriostatic ability and bacteria excretion are poor. Parents
who are nursing a sick child will often wipe the child’s tears
away, which can lead to infection caused by conditional
pathogenic bacteria and local suppurative infection.
Usha
(23) reported the sensitivity of G+ and G− bacteria
to levofloxacin as 75% and 83%, respectively. The
sensitivities of Gram-positive and Gram-negative bacteria
to levofloxacin, as reported by Sun
(22), were 83.91% and
93.33%, respectively. Our results show that levofloxacin
has become the most sensitive antibiotic for children with
dacryocystitis, with an average efficacy rate of 96.81%. Thus,
we believe that levofloxacin ophthalmic gel is the agent
of choice for combination therapy with nasolacrimal duct
probing.
According to our findings, the 1-time success rate of
traditional nasolacrimal duct probing in the 3–6 months age
group was 95.65% and that in the 7–12 months age group was
88.24%, which is slightly higher than the findings by Lipiec
(24) (83% and 71%, respectively) and lower than those reported by
Perveen
(25) (100% and 94%, respectively). The 1-time success
rate in the 7–12 months age group in our study is higher than
that reported by Repka
(13) (78%). The 1-time success rate
of nasolacrimal duct probing for children from 3–6 months
of age is generally higher than the rate for those older than
6 months. Therefore, the first nasolacrimal duct probing
(27) should be performed in children from 3–6 months of age.
The lower success rate in children older than 6 months
of age compared to children younger than 6 months is likely
because children older than 6 months cry harder under
local anesthesia, the duration of the procedure may cause
greater tissue damage, and tissue proliferation
may reduce
the effectiveness of probing. However, some scholars
(27) have suggested that inflammation did not promote the
proliferation at the obstruction. Whether or not proliferation
occurs, traditional nasolacrimal duct probing may inevitably
cause mucosa edema of the lacrimal duct and even injury
to mucosal epithelial cells. If inflammation lasts for a long
time and postoperative tissue edema and reaction are severe,
re-adhesion and obstruction may occur. Thus, the 1-time
success rate in children older than 6 months is lower than
those younger than 6 months.
We found that combining nasolacrimal duct injection
of levofloxacin ophthalmic gel with probing significantly
improves the 1-time success rate over probing alone in
children aged over 6 months, from 88.24% to 96.52%.
Levofloxacin
(28) is a third-generation fluoroquinolones
that has fewer side effects. It kills bacteria by inhibiting
their DNA gyrase action and blocking DNA reproduction.
According to our results as well as previous studies, the
vast majority of G+ and G− bacteria exhibit a high rate of
sensitivity to levofloxacin.
Another advantage of levofloxacin ophthalmic gel is that
its soft, gelatinous consistency is released slowly, thereby
prolonging the duration of drug action. The main substrates
are sodium hyaluronate and carbomer, the latter of which
is characterized by high viscosity and good lubrication.
Carbomer forms a protective film on the surface of
nasolacrimal duct tissues. Sodium hyaluronate plays a role
in expanding, supporting, and separating mucosal wounds
and lubricating the application site. The degradation and
liquification rates are rapid and will not cause residuals. One
study supported the use of levofloxacin ophthalmic gel
(29). Due to its strong bioadhesion, it may facilitate formation of
a protective film on the surface of nasolacrimal duct tissues
after probing and irrigation.
Congenital dacryostenosis
(30) is a common condition
in which the far end of the nasolacrimal duct underneath
the inferior turbinate and epithelial cell debris blocking
fails to complete its canalization in the newborn period. As
the duration of the obstruction increases, serious infective
complications occur. Inflammatory reaction can cause
edema and hyperplasia and stimulate epithelial hyperplasia.
If inflammation lasts for a long time and postoperative tissue
edema and reaction are severe, re-adhesion and obstruction
may occur. And in 3–6 month group, the duration of
the inflammatory reaction was shorter the chance of readhesion
after valve probing was low. Therefore, the
support function of the gel is not needed. So the 1-time
success rates of combination with levofloxacin ophthalmic
gel or not showed no different in 3–6 month group.
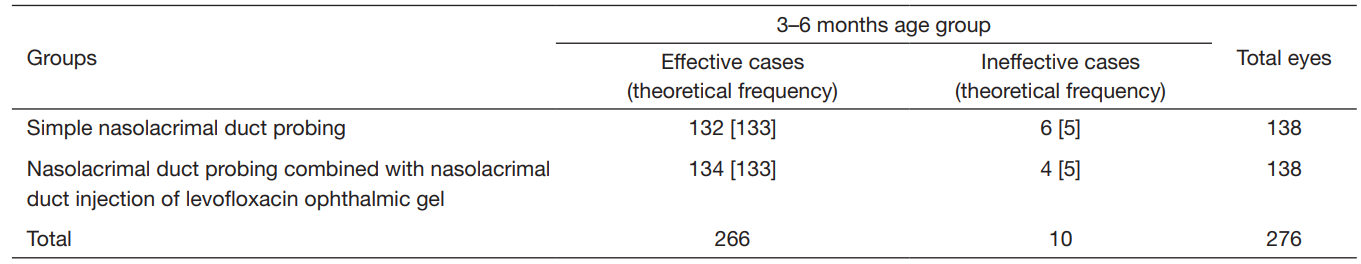
Table 2 Comparison of curative effect of two treatment methods in 3–6 months age group
χ2 =0.104, P=0.747>0.05; the difference had no statistical significance.
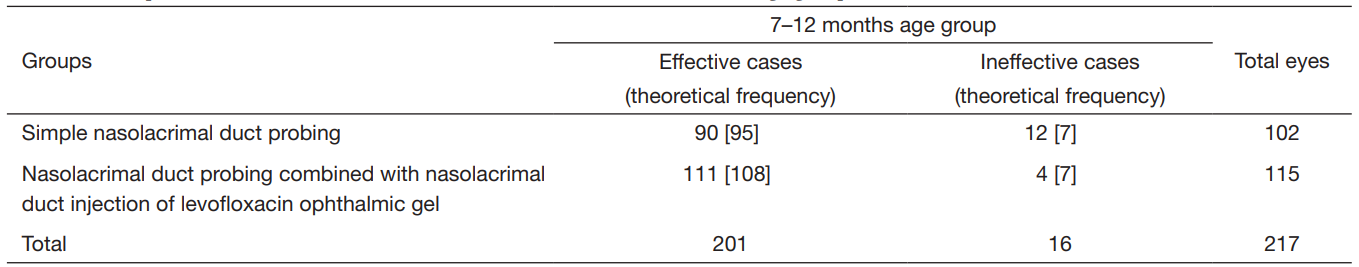
Table 3 Comparison of curative effect of two treatment methods in 7–12 months age group
χ2=5.435, P=0.02<0.05; the difference had statistical significance.
Table 4 Curative effect of simple nasolacrimal duct probing in different age groups
χ2=4.651, P=0.031<0.05; the difference had statistical significance.
Table 5 Curative effect of nasolacrimal duct probing combined with nasolacrimal duct injection of levofloxacin ophthalmic gel in different age groups
χ2=0.000, P=1.000>0.05; the difference had no statistical significance.
Conclusions
For children from 7–12 months of age, nasolacrimal duct
probing combined with nasolacrimal duct injection of
levofloxacin ophthalmic gel may increase the 1-time success
rate of treatment.