Using a +20D lens for non-contact slit lamp biomicroscopy of ocular fundus
来源期刊: 眼科学报 |
2016年9月 第31卷 第3期: |
192-194
发布时间:
收稿时间:2024/11/30 20:53:55
阅读量:948
- 作者:
-
- 关键词:
-
-
- DOI:
-
doi: 10.3978/j.issn.1000-4432.2016.09.04
- 收稿时间:
-
2016-07-29
- 修订日期:
-
- 接收日期:
-
2016-08-31
Noncontact slit lamp examination of the ocular fundus has
been classically done using high power convex lenses like
+90D, +78D, and +60D. A real and inverted image of the
fundus is formed in between the high power convex lens and
the slit lamp. The +20D lens is commonly used for binocular
indirect ophthalmoscopy. The authors use this +20D lens for
slit lamp biomicroscopy examination of the fundus.
An informed consent of the patient for a clinical
examination is obtained. Unlike the contac t lens
biomicroscopic examination, corneal anesthesia and
coupling gel is not required. The pupil is dilated
maximally. The eye is made stable by using the fixation
of the eye being examined or the contralateral eye. Both
the examiner and the patient are seated comfortably at
the slit lamp. The magnification of the biomicroscope is
kept at the minimum. The width of the slit lamp beam
is decreased to avoid reflections. The patient shifts chin
back (away from the headband) on the chin rest. At
this position, the patient’s forehead does not touch the
headband (Figure 1A, red arrow). The +20D lens is held
near the headband (Figure 1A). With coaxial illumination,
the joystick of the slit map is moved away from the
headband until a clear image of the fundus is obtained.
Most of the times, the joystick needs to be moved fully
back to get a proper image (Figure 1A, green star).
Magnified stereoscopic view of the fundus is possible
with the method (Figure 1B,C). Troublesome reflections
may be prevented by making the light source slightly off -
axis. With practice, examination of fundus up to equator is
possible by moving the eye.
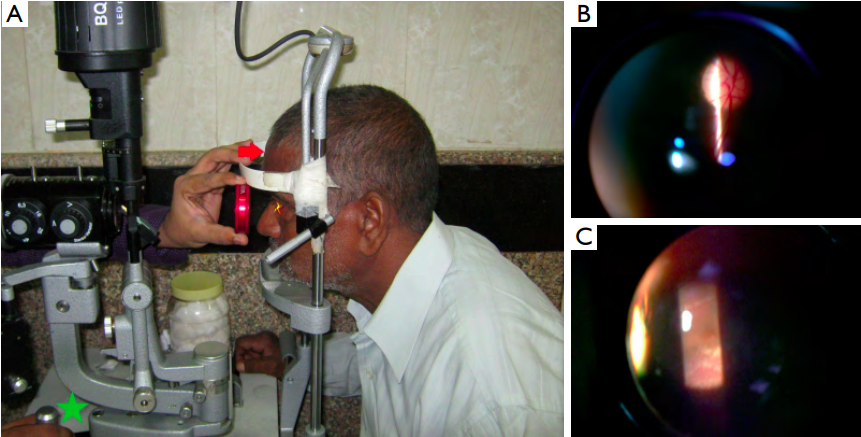
Figure 1 Examination of the fundus on slit-lamp using a +20D lens. (A) The patient’s head is positioned away from the headband (red arrow)
and the joystick is drawn fully back from the headband toward the examiner (green star). The slit lamp is kept co-axial; (B) stereoscopic
examination of the optic disc is shown; (C) the foveal depression along with minute details can be evaluated though annoying reff exes need
to be avoided.
Examination of the fundus may be achieved by negating the converging refractive apparatus of the
eye (erect, virtual image) or by adding a convex lens
to this converging refractive apparatus in an indirect
ophthalmoscopic examination (inverted, real image).
The rays originating from the retina of an emmetropic
eye are parallel after emerging from the cornea. Thus,
the image of the retina formed by the condensing lens
used for indirect ophthalmoscopy lies at the focal plane
of the lens. For a +20D lens with a lens diameter of 25
and 40 cm, the distance from the cornea to the lens is 6
and 5.6 cm respectively (1). The image is formed at the
focal plane at 5 cm from the +20D lens on the side of the
examiner. Thus, for viewing the inverted real image of the
patient’s fundus through a slit lamp with a +20D lens of
25 or 40 cm diameter, the patient’s cornea should be 11
or 10.6 cm farther than the focal point of the slit lamp
microscope. To provide this increased distance, the slit
lamp has to be brought maximally to the examiner as
well as the patient has to shift his head away from the
headband.
Gellrich MM used various plus lenses (+20D, +40D,
+55D, +60D, and +90D) for slit lamp biomicroscopy of
the fundus (2). He noted that the problems with +20D
lens were the need of increased examination distance over
10 cm and increased intensity of light over the fundus.
Light-induced maculopathy is a potential concern for slit
lamp biomicroscopy of the fovea using any lens and even
anterior segment (2,3). Kohnen reported two pseudophakic
patients with visual acuity of 20/25 who worsened to
hand movements following slit lamp photography of the
anterior segment for documentation of posterior capsule using retroillumination (3). The slit lamp used Xenon
lamp as the light source, and the exposure may have been
more than 10 minutes especially during the adjustments.
Both patients noted vision loss immediately after the slit
lamp photography. One patient reported pain during the
photography, and both patients showed multiple macular
scars simulating laser burns (3).
The angle between the observation system and
the illumination system should be very small during
use of a low-power plus lens (2). Other limitations of
this technique include the need for maximal pupillary
dilatation and patient cooperation. Also, it is not easy to
see the peripheral retina using this technique. Annoying
reff exes may obscure the image and positioning the patient
may be difff cult. Beginners may require 3–5 minutes to get
a sharp image of the fundus when using +20D for the ff rst
time in slit lamp. The static field of view is smaller and
magnification is more compared to the +90D lens. With
full pupillary dilation approximately 10º–15º of fundus can
be visualized in a single field.
Media haze (corneal opacity, cataract, asteroid hyalosis,
synchysis scintillans) and high magnification also may
degrade the image quality of the fundus. We have
examined more than 100 patients using this method,
and we have not noted any specific side effects so far.
We believe the stereoscopic appreciation of contour of fovea may be better than +90D when the examiner is
accustomed to the technique. Positioning the patient and
avoiding the reff exes are the most important skills which a
beginner takes time to master. However, in areas with lack
of resources, a single +20D lens can be very useful for both
indirect ophthalmoscopy and a stereoscopic evaluation of
the posterior pole.
1、Colenbrander A. Chapter 63: Principles of Ophthalmoscopy. In: Tasman W, Jaeger EA. editors. Duane’s Clinical Ophthalmology on CD-ROM. Vol 1. Philadelphia: LWW, 2004. Available online: http://www.oculist.net/downaton502/prof/ebook/duanes/pages/v1/v1c063.html, accessed 5th September 2016.
2、Gellrich MM. The fundus slit lamp. Springerplus 2015;4:56.
3、Kohnen S. Light-induced damage of the retina through slit-lamp photography. Graefes Arch Clin Exp Ophthalmol 2000;238:956-9.