Examination results of all the students from the theoretical
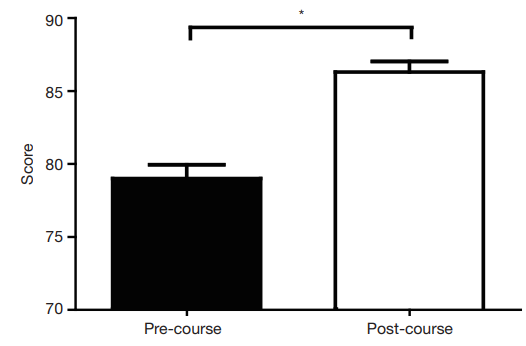
course and the clerkship were collected and analysed. Postcourse
results (range from 60 to 93.5; mean score 86.3000;
standard deviation 5.8146) were significantly higher than
pre-course results (range from 72 to 100; mean score
79.0079; standard deviation 7.5169) (mean increase of 7.29;
95% confidence interval, 5.18-9.41;
<0.0001) (Figure 3).
The gap between high scores and low scores was narrow.
Forty-nine students (77.78%) gained ophthalmic knowledge
and learned skills to different degrees (10.59±6.20).
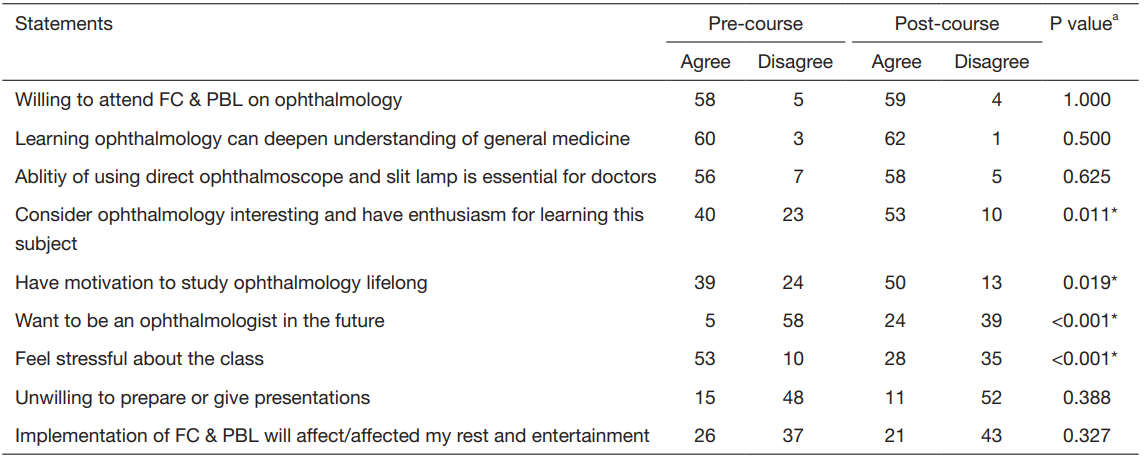
The statements on the pre-course questionnaire were
designed to establish a baseline of the students’ attitudes
and preferences before class (Table 1). The majority of
students were willing to participate in FC & PBL and
quite optimistic about learning ophthalmology before
class. Thirty-nine (61.90%) students agreed and strongly
agreed that they had motivation to study ophthalmology
throughout their life, but only 5 (7.94%) students wanted
to be ophthalmologists. Responses to questions 7 through 9
indicated that a certain number of students felt stressful and
reluctant to do the presentations and were afraid that the
implementation of FC & PBL would disturb their daily life.
Comparison of pre-and post-course questionnaires
indicated remarkable changes in four questions. After
class, the interest and motivation to study ophthalmology
increased, and 24 (38.10%)students expressed desires to be
eye doctors, which is significantly higher than pre-course responses. Additionally, the number of students that felt
stressful about the class reduced.
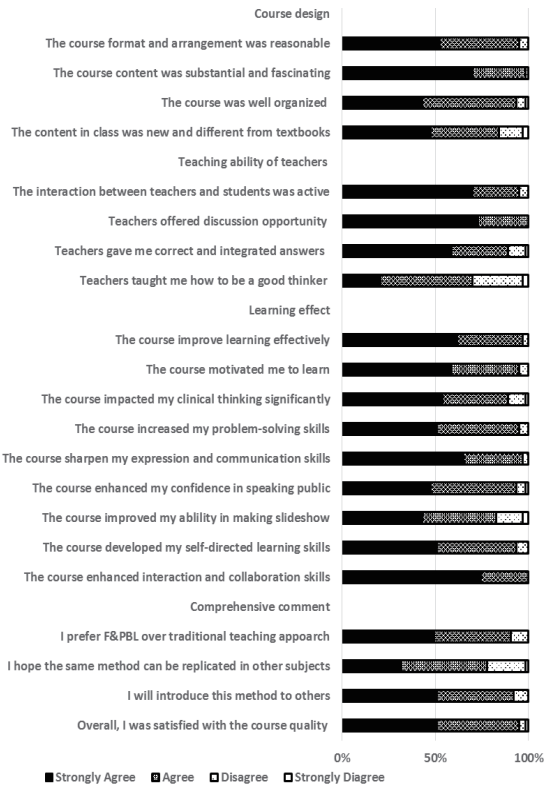
The 21 additional post-course questions were set up
to have a deeper insight into the influence of FC & PBL
on the learning experience, including course design, the
teaching ability of the teachers, the learning effect and
comprehensive comments (Figure 2). All of the statements
received more than 50% positive responses. Most of the
students were satisffed with the course design and teachers’
teaching abilities.
For the learning effect perception, students strongly
agreed or agreed that the course improved learning
knowledge effectively (n=61, 96.83%), motivated students
to learn (n=60, 95.24%), impacted clinical thinking
signiffcantly (n=56, 88.89%) and increased problem-solving
skills (n=60, 95.24%). Of the 63 respondents, 57 (90.48%)
participants preferred the FC & PBL model over the
traditional course format, and 95.24% were satisfied with
the quality of the course. All students strongly agreed or
agreed that teachers offered opportunities for discussion
and the course enhanced interaction and collaboration skills
immensely. However, perceptions on “teachers taught me
how to be a good thinker” and “I hope the same method can
be replicated in other subjects” had relatively less positive
responses, but the number of strongly agree and agree still
accounted for more than half of respondents.
In the open-ended section for suggestions and feelings,
majority of students considered the new method in
ophthalmology clerkship fresh and attractive. Students
spent a lot more time preparing than in the traditional
class, but the rewards were greater. Whereas some students
argued that they were incapable of finding satisfying
answers. A part of students suggested that the process could
be slower so that they could grasp the core concepts more
clearly. Another suggestion was that more communication
with teachers was needed outside of the classroom.
Table 1 Comparison of pre-course and post-course perception on FC & PBL (n=63)
a , exact McNemar’s test;
*,
statistical significance; FC & PBL, flipped classroom and problem-based learning.
Discussion
The results of current study show that utilizing FC and PBL
increased students’ knowledge and produce more positive
attitudes towards ophthalmology. We were delighted to
see that the number of students that now aspire to be eye
doctors markedly increased after the clerkship.
The advantages of FC and PBL have been revealed in
this study. The post-course examination contained casebased
problems, and the improved results demonstrated the
students’ comprehension of clinical analysis and knowledge application. Although most students were satisfied with
this study, some students were not. Some students did not
understand the class well and had low efficiency in their
searches for satisfactory answers, which might due to their
unfamiliarity with active learning modules. Some of them
wished to have communication with teachers. Hence, it is
necessary to promote active learning methods in medical
education and teachers have to put more effort into
interactions with students.
Ophthalmology is a relatively underrepresented
medical specialty. As such, little effort has been put into
the curriculum by educational institutions and students.
Combined with traditional didactic teaching models,
students’ passion for learning ophthalmology is relatively
nonexistent. Both FC and PBL are feasible ways to reverse
the declining trend of ophthalmology education
(5,8,11,12).
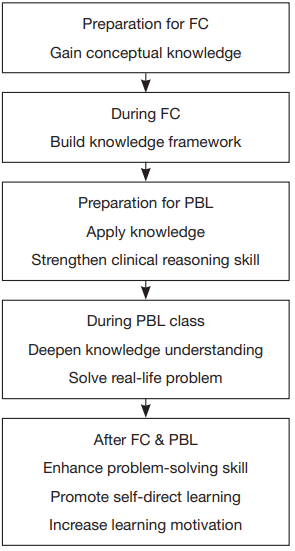
In FC, students study independently to gain conceptual
knowledge. In-class teaching is based on teacher-student
interactions instead of one-way lecturing, which leads to
greater student engagement, enhanced motivation to learn,
more positive attitudes, and better relationships between
teachers and students
(13). PBL is another active learning
approach. Preparation for PBL is a process of applying
knowledge and strengthening clinical reasoning skills. In
this manner, students learn about a subject by exploring an
unstructured topic. Moreover, it emphasizes the application
of theoretical knowledge to solve problems in the real
world. Students are allowed to stage a debate during the
class, where they have to articulate their thoughts and
develop arguments to support their views. Communication,
problem-solving, and critical-thinking skills are fostered in
the process.
Nevertheless, some educators argue that PBL is
not better than traditional teaching methodologies
in improving learning outcomes. This may be due to
student unfamiliarity with the new module or inadequate
understanding of basic concepts
(14,15). Adopting a
FC to facilitate conceptual framework formation is an
optimal solution for this problem. Until now, educators
understood that integrating a FC and PBL was a possibility,
but few studies document the combination. These two
methodologies share an emphasis on higher order thinking
skills, and are used in conjunction with one another. That
is, they are complementary. Using FC&PBL maximizes
class time and allows students to learn individually or
through group activities. Without PBL, students put less
effort into understanding concepts, and they do not learn
how to handle real life problems. Likewise, implementing
PBL without FC module will require too much class time
for teaching and learning to be able to apply the knowledge.
The FC provides a promising framework of knowledge for
PBL instruction, which promotes information retention.
Meanwhile, because ophthalmology is a visual science
and ophthalmologists make judgements on visual
characteristics, we applied clinical cases, real patients, and
slit-lamp multimedia systems as subsidiary strategies to
improve class quality
(16). Besides, we used ocular trauma
as the major content of case discussions. Ocular trauma is an ophthalmic emergency that needs considerable attention.
It is a preferable discussion topic due to its complexity and
various clinical features. Clinical images of ocular traumas
are available to show different signs, so students can see
exactly what the clinical features look like. Multimedia
systems can assist teachers in demonstrating the dynamic
changes from real patients, such as iridodonesis.
There were several limitations in our study. First, the
PBL team size was large, thus few students had frequent
chances to make statements or communicate with others.
Second, because the teaching faculty had to pay attention
to everyone’s performance, not receiving enough individual
attention may have negatively affected some students’
attitudes. Third, as the participants were voluntarily taking
part in our study, the willingness of active learning might
influence the teaching outcome and we cannot evaluate
the effect among the less initiative students. Fourth, there
was not a control group to compare the effectiveness of
the format, due to ethical problems and time constraints.
Further studies and investigations are required that include
a control group to obtain a better understanding of this
methodology. Additionally, it might take a lot of time for
students to prepare the class, and further and more extensive
studies would find out the practicality of these approaches.
Another limitation was that some sections like diabetic
retinopathy and age-related macular degeneration were not
included in our study, and we will add these sections in the
future study.
Conclusions
The study is a preliminary attempt to integrate the FC
and PBL approaches in ophthalmology education. This
relatively cost-effective methodology provides an engaging
and active learning environment where students can gain
ophthalmic knowledge, clinical skills, problem-solving
abilities, self-directed learning abilities, and motivations.
All of these elements contribute to the lifelong professional
growth of medical students and can assist in their future
careers.