Twenty-seven patients (30 eyes) were enrolled and completed
the operation; mitomycin C was used on ten eyes. All patients
were followed up for at least 12 months. The preoperative
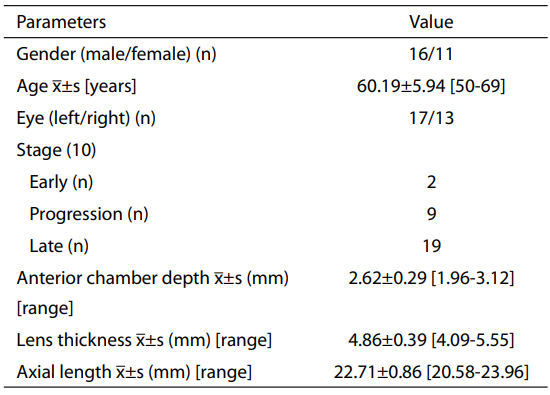
information of the enrolled patients is shown in Table 1.
Table 1 Preoperative general information of the enrolled patients
Visual acuity, IOP, and visual field
No significant decrease in visual acuity was observed at
days 1 and 7 and at months 1, 3, 6, and 12 after operation
(
P>0.05); however, a significant decrease in IOP was
observed at days 1 and 7 and at months 1, 3, 6, and 12 after
operation (
P<0.01). Moreover, no significant progression
in visual field mean defect was observed at months 6 and 12
after operation (
P>0.05) (Table 2).
Table 2 Change in visual acuity, IOP, visual fi eld, and medications before and after operation (x±s) (n=30)
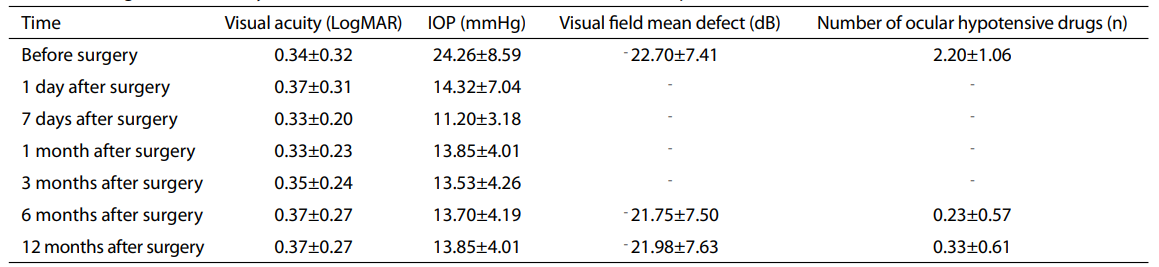 IOP, intraocular pressure.
IOP, intraocular pressure.
Use of ocular hypotensive drugs
Before operation, 30 eyes (100%) required the use of ocular
hypotensive drugs. At month 6 after operation, four eyes
(13.33%) required the use of ocular hypotensive drugs, and
at month 12 after operation, seven eyes (23.33%) required
the use of ocular hypotensive drugs. The number of ocular
hypotensive drugs required was significantly reduced at
months 6 and 12 after operation (
P<0.05). More ocular
hypotensive drugs were required at month 12 after operation
than at month 6 after operation, but the difference was not
statistically significant (
P>0.05) (Tables 2,3).
Table 3 The number of ocular hypotensive drugs used before and after operation (n=30)
Intraoperative cooperation
All operations were successfully completed under topical
anesthesia; among these, 13.3% (4/30) of operations
required additional topical anesthesia. Patient-rated
anesthetic effect was 0.53±1.02 (range, 0-3.0). Surgeonrated
patient cooperation was “good” (86.7%, 26/30) and
“fair” (13.3%, 4/30).
Intraoperative complications
No intraoperative complications were observed.
Postoperative inflammatory response of the anterior
chamber
All 30 eyes are in mild response.
Postoperative complications
During the first week after operation, four eyes (13.3%)
exhibited shallowing of the anterior chamber (not reaching
shallow I), which improved 2-4 days after the dosing of 1%
prednisolone acetate eye drops was adjusted to 3-4 times/day;
one eye (3.33%) exhibited conjunctival flap leakage and
shallow anterior chamber (shallow I). The anterior chamber
depth returned to normal after a soft bandage contact lens
was worn for 3 days; the contact lens was removed 7 days
later, and no incision leakage was observed. Three eyes
(10%) exhibited IOP >21 mmHg during the first week after
operation, during which one eye underwent laser removal
of scleral stitches, and two eye received massage. IOP
was under control. No complications (such as malignant
glaucoma, choroidal detachment, or filtering bleb infection)
were observed.
Filtering blebs
At month 12 after operation, 13.33% (4/30), 83.33%
(25/30), 3.33% (1/30), and 0% (0/30) of eyes were of types I,
II, III, and IV, respectively.
Surgical success rate
At month 6 after operation, the surgical success rate was
86.7% (26/30), and the overall success rate was 93.33%
(28/30); at month 12 after operation, the surgical success
rate was 76.67% (23/30), and the overall success rate was
93.33% (28/30). No significant difference was observed
in the surgical success rate between months 6 and 12 after
operation (
χ2 =1.47,
P=0.48).
Discussion
In this study, we introduced minimally invasive
trabeculectomy to minimize tissue damage in the surgical
field during trabeculectomy. All patients in this study
successfully underwent operation under topical anesthesia
without the need for sutures to fix the eye. Moreover,
patient-rated anesthesia was good, suggesting that
topical anesthesia was safe and feasible while minimizing
pain. In addition, we used a trabecular cutter during the
operation for the precise resection of trabecular tissue.
While replacing the iris, we advantageously used a scleral
flap rather than an iris replacer, which helped to reduce
postoperative inflammation. Consequently, only mild
infl ammation was observed after operation.
Patients enrolled in this study had angle-closure
glaucoma that was characterized by a shallow anterior
chamber, thick lens and short axial length. Using watertight
scleral sutures and intraoperative reconstruction of the
anterior chamber, during operation and the fi rst week after
operation, four eyes (12.5%) exhibited shallowing of the
anterior chamber (not reaching shallow I) that was resolved,
and one eye (3.12%) had conjunctival flap leakage and
shallow anterior chamber (shallow I) that recovered after
wearing a soft bandage contact lens. Thus, the incidence of
complications was lower than that reported by Edmunds
et al. (15), where the incidence of intraoperative bleeding
in the anterior chamber, postoperative shallow anterior
chamber, and conjunctival flap leakage was 24.6%, 23.9%,
and 17.8%, respectively. Moreover, in this study, no other
complications (such as malignant glaucoma, choroidal
detachment and endophthalmitis) were observed, suggesting
that the modifi ed procedure is safe for PCACG and reduces
the incidence of postoperative complications, such as
shallow anterior chamber and low IOP.
In this study, during the first week after operation,
three eyes (10.52%) exhibited IOP >21 mmHg and this
was primarily due to tight scleral sutures. Specifically, one
eye underwent laser removal of scleral sutures, and two
eyes received massage. Consequently, IOP was rapidly
controlled. However, two eyes exhibited long-term high
IOP, suggesting that it is important to avoid tight sutures
during operation and that patients with elevated IOP during the early stage after operation should be closely monitored
and receive interventions if needed to ensure long-term
treatment outcome.
In this study, we used less invasive surgical approaches
and instruments, such as non-invasive forceps and trabecular
cutters, to reduce surgical damage(16); we used topical
anesthesia to avoid complications that are associated with
postbulbar anesthesia or beneath-the-fascia anesthesia(11);
to reduce eye muscle or corneal damage, we did not use
sutures to fi x the eye; we used non-invasive forceps to grip
the conjunctiva with a smaller conjunctival flap and reduce
conjunctival damage; we used thermal hemostasis with
a hemostatic sponge to mitigate the thermal reaction of
the scleral surface caused by direct burning; and we used
a scleral tunnel scalpel to make a (smaller) scleral flap to
reduce damage to the scleral tissue and the surrounding
vessels, thereby reducing the wound healing response of
ff ltration surgery and postoperative scarring and facilitating
the establishment of good filtration pathways (17). In this
study, at month 12 after operation, 83.33% of the operated
eyes had type II filtering blebs, and 96.67% (29/30) had
a functional bleb morphology. No complications (such as
filtering bleb infection) were observed.
In this study, the patients were followed up for at least
1 year, and no significant decrease in visual acuity was
observed after operation; IOP was signifi cantly reduced after
operation, no signifi cant progression was observed in visual
ff eld mean defect at months 6 and 12 after operation, and the
number of ocular hypotensive drugs used was significantly
reduced at months 6 and 12 after operation. The surgical
success rate observed was higher than that reported by
Edmunds et al. (18), who reported a 1-year absolute surgical
success rate of 66.6% and an overall success rate of 71.0%.
Collectively, these findings suggest that our modified
procedure improved the surgical success rate.In this study,
some patients required ocular hypotensive drugs at months 6
and 12 after operation, mainly because these patients had
advanced visual field changes caused by glaucoma before
operation, thus requiring a lower IOP target.
This study has some limitations, including small sample
size, short follow-up time, and lack of a suitable control.
In future studies, we will enroll more patients and use a
longer-term follow-up period to further investigate longterm
IOP management after operation.